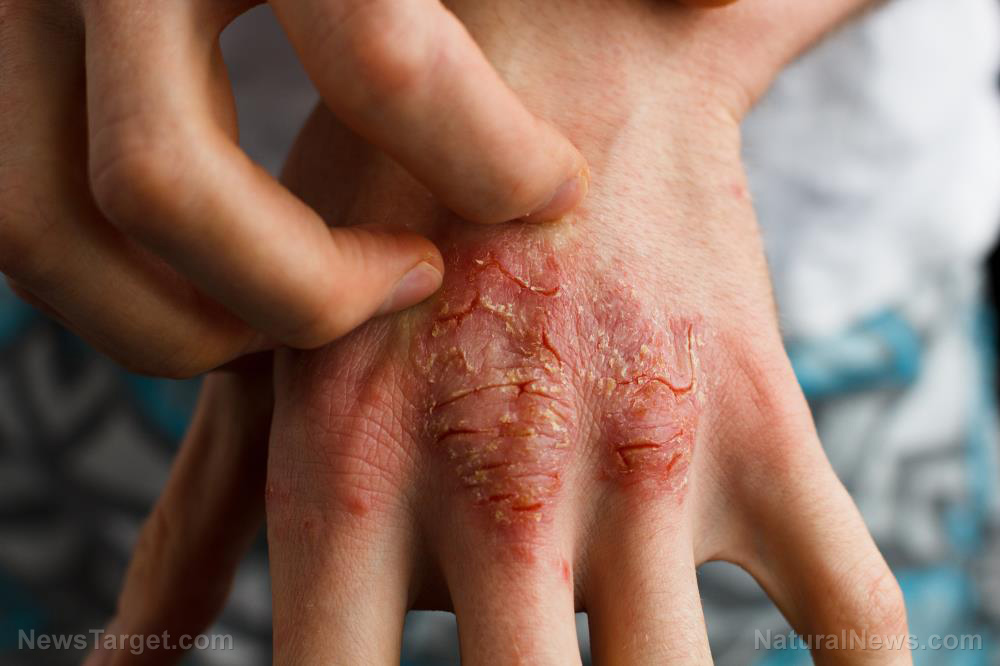
Atopic Dermatitis Increases Global Risk of Asthma and Rhinitis
A recent global analysis published in the European Medical Journal reveals that individuals with atopic dermatitis face a significantly higher risk of developing respiratory conditions like asthma and rhinitis, reinforcing the 'atopic march' concept. India shows some of the highest rates of these comorbidities. This research highlights the critical need for integrated clinical management and public health strategies worldwide.
Key Highlights
- Atopic dermatitis significantly elevates the global risk of asthma and rhinitis.
- Study provides the first standardized worldwide estimates of these comorbidities.
- Global prevalence of asthma in AD patients is 20.1%, and rhinitis is 45.1%.
- Patients with AD are nearly three times more likely to develop asthma.
- India shows one of the highest comorbidity rates, with up to 59.4% for asthma.
- Findings reinforce the 'atopic march' progression from skin to respiratory allergies.
A significant global analysis, summarized by the European Medical Journal, highlights a strong and consistent link between atopic dermatitis (AD) and a substantially increased risk of developing respiratory comorbidities such as asthma and rhinitis. This extensive review and modeling effort provides the first standardized worldwide estimates of these co-occurring conditions, underscoring important implications for both clinical management and global public health planning.
The study, originally published in the British Journal of Dermatology on February 5, 2026, systematically reviewed 278 studies and utilized a hierarchical Bayesian model to generate comprehensive global, regional, and country-level estimates of respiratory disease burden in individuals affected by AD. The findings reveal that globally, approximately one in five individuals with AD also suffers from asthma, with an estimated prevalence of 20.1%. Rhinitis, an inflammation of the nasal lining, was found to be even more prevalent, affecting 45.1% of AD patients. More specifically, allergic rhinitis was reported in 41.4% of cases, and rhinoconjunctivitis (which includes eye symptoms) in 30.7%. A considerable 10.4% of people living with AD experience both asthma and rhinitis simultaneously.
Crucially, the research demonstrates that individuals with atopic dermatitis are at a significantly higher risk of developing these respiratory conditions compared to those without the skin condition. The odds of developing asthma were found to be nearly three times higher in AD patients, while the risk for rhinitis and rhinoconjunctivitis was similarly elevated. These elevated risks emphasize the systemic nature of atopic diseases, which are characterized by an overactive immune response.
The analysis also brought to light substantial geographical variations in the prevalence rates of these comorbidities. For instance, the prevalence of asthma among AD patients ranged dramatically from a low of 2.5% in Israel to nearly 60% in India. Similarly, rhinitis prevalence in AD patients varied from 7.8% in Israel to an alarming 82.7% in India. India, alongside Cuba, Finland, and Puerto Rico, was identified as having some of the highest observed comorbid prevalence rates, suggesting that environmental, genetic, or healthcare-related factors may play a significant role in influencing disease expression across different regions. For an Indian audience, these statistics are particularly relevant, highlighting a significant public health challenge within the country.
These findings strongly reinforce the well-established concept of the 'atopic march' (also known as the 'allergic march'). The atopic march describes a natural progression of allergic diseases that typically begins in infancy with atopic dermatitis (eczema), followed by the development of food allergies, and subsequently respiratory allergies such as allergic rhinitis (hay fever) and asthma later in childhood or adolescence. This temporal sequence suggests a shared underlying immune dysregulation, often involving IgE antibody responses to common allergens. The disrupted skin barrier in atopic dermatitis is believed to be a critical initial step, potentially leading to increased sensitization to allergens through the skin, which can then predispose individuals to developing respiratory allergies.
While the concept of the atopic march is widely acknowledged, some research suggests the causal link may be more complex than a simple linear progression in every individual, proposing it might be better understood as a population-level phenomenon rather than an absolute individual trajectory. Nevertheless, the observed strong associations and increased risks are undeniable, necessitating a comprehensive approach to managing these interconnected conditions. The study highlights the importance of accurate clinical assessment, noting that prevalence estimates were generally higher when AD diagnoses were confirmed by dermatologists or physicians.
Understanding this complex relationship is crucial for developing early preventative and management strategies. The burden of atopic diseases, including atopic dermatitis, asthma, and allergic rhinitis, affects a substantial portion of the global population, with estimates suggesting up to 20% of the world's population is affected by atopic conditions. Atopic dermatitis alone is a leading contributor to the global burden of skin disease, affecting an estimated 230 million people, while asthma affects nearly 340 million people worldwide. The economic burden associated with these chronic conditions is also substantial.
This research emphasizes the need for healthcare providers, particularly in regions with high comorbidity rates like India, to screen individuals with atopic dermatitis for potential respiratory complications. Early identification and integrated management strategies could significantly improve patient outcomes and reduce the overall burden of these diseases. The study serves as a vital resource for informing clinical guidelines and public health policies aimed at addressing the intertwined nature of atopic conditions on a global scale.
Frequently Asked Questions
What is the 'atopic march' and how does it relate to atopic dermatitis?
The 'atopic march' describes the typical progression of allergic diseases, often starting with atopic dermatitis (eczema) in infancy. This can then be followed by the development of food allergies, and later, respiratory allergies such as allergic rhinitis and asthma. It highlights the interconnected nature of these conditions, often driven by shared immune system dysregulation.
How much higher is the risk of asthma and rhinitis for people with atopic dermatitis?
Globally, individuals with atopic dermatitis have nearly three times higher odds of developing asthma compared to those without the skin condition. The risk for rhinitis and rhinoconjunctivitis is similarly elevated. The global prevalence of asthma in AD patients is estimated at 20.1%, and for rhinitis, it's 45.1%.
Why is this research particularly relevant for India?
The global analysis indicates that India has one of the highest observed comorbid prevalence rates of asthma and rhinitis in individuals with atopic dermatitis. For example, asthma prevalence in AD patients in India can be as high as 59.4%, and rhinitis as high as 82.7%, significantly impacting public health in the country.
What are the implications of these findings for patient care?
These findings emphasize the importance of integrated clinical management. Healthcare providers should consider screening individuals with atopic dermatitis for potential respiratory comorbidities like asthma and rhinitis. Early diagnosis and a holistic approach to managing these interconnected conditions can lead to improved patient outcomes and quality of life.
Is the link between atopic dermatitis and respiratory allergies definitively causal?
While the strong association and increased risk are well-established, some researchers suggest that the 'atopic march' may reflect a population-level phenomenon rather than a strict causal progression in every individual. However, the evidence for a significant link and shared immunological pathways is robust, making the association clinically important.